Every movement your child makes — from taking first steps and climbing stairs to smiling and holding a spoon — depends on healthy nerves and muscles working together. However, when this system is affected, everyday tasks can become more difficult. These conditions are known as neuromuscular disorders, and they can cause symptoms such as weakness, poor balance, fatigue, or trouble with breathing and swallowing. Fortunately, with early diagnosis, the right therapy, and family support, many children can make meaningful progress and enjoy a better quality of life.
What Are Neuromuscular Disorders?
If you are asking what are neuromuscular disorders, it is a broad group of conditions that affect the peripheral nerves, muscles, or the communication between nerves and muscles. As a result, the body may have difficulty with movement, balance, coordination, or strength. Common effects include muscle weakness, muscle wasting, reduced reflexes, pain, numbness, or sensory changes.
There are many different types, ranging from mild to progressive conditions. For example, spinal muscular atrophy (SMA) affects approximately 1 in 6,000 to 10,000 live births. Therefore, early diagnosis, therapy, and neurodevelopmental support can help improve daily function and quality of life.

Types of Neuromuscular Disorders
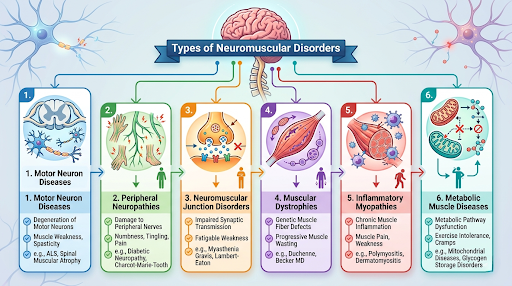
Many conditions fall under this category. To understand them better helps families know where symptoms may begin and what care may be needed.
1. Motor Neuron Diseases
These affect nerve cells that control movement. Examples include ALS, Spinal Muscular Atrophy (SMA), and Polio. In children, SMA is especially important because it can affect early development.
2. Peripheral Neuropathies
These involve nerves outside the brain and spinal cord. Because of this, children or adults may feel weakness, numbness, or pain. Examples include Guillain-Barré syndrome, diabetic neuropathy, and Charcot-Marie-Tooth disease.
3. Neuromuscular Junction Disorders
These happen when signals between the nerve and muscle are disrupted. As a result, muscles may tire easily or become weak. Examples include Myasthenia Gravis and Lambert-Eaton syndrome.
4. Muscular Dystrophies
These are genetic conditions that cause progressive muscle breakdown. Duchenne muscular dystrophy often begins in childhood. Other forms include Becker and Limb-Girdle muscular dystrophy.
5. Inflammatory Myopathies
These are autoimmune muscle diseases where the immune system attacks healthy muscle tissue. Examples include Polymyositis, Dermatomyositis, and Inclusion Body Myositis.
6. Metabolic Muscle Diseases
These develop when the body cannot create or use muscle energy properly. For example, Pompe disease and some glycogen storage diseases belong to this group.
Symptoms
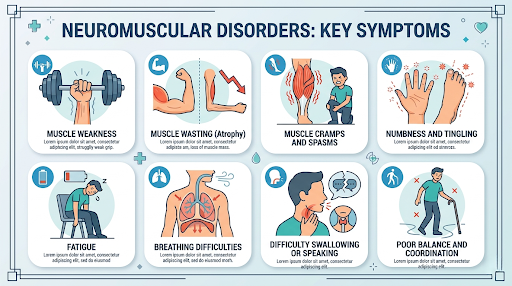
Recognizing neuromuscular disorders symptoms early can help families seek support sooner and begin the right treatment plan.
Muscle Weakness — The most common sign. A child may struggle to walk, climb stairs, lift toys, or hold objects.
Muscle Wasting (Atrophy) — Muscles may become smaller over time because they are not working normally.
Muscle Cramps and Spasms — Painful tightening or involuntary movements can happen in some conditions.
Numbness and Tingling — Often felt in the hands or feet when nerves are involved.
Fatigue — Unusual tiredness may appear even after light activity.
Breathing Difficulties — In more severe cases, chest muscles may become weak.
Difficulty Swallowing or Speaking — Facial, throat, or tongue muscles may be affected.
Poor Balance and Coordination — Children may appear clumsy, unstable, or fall often.
Early Signs in Children
In children, early signs may include delayed sitting, frequent falls, toe walking, or trouble rising from the floor. If these symptoms continue, a specialist assessment is important.
Neuromuscular Disorder ICD 10 Codes
For medical documentation and insurance purposes, these conditions are classified under specific ICD-10 codes. In addition, knowing the right neuromuscular disorder ICD 10 category can help with referrals, records, and therapy approvals.
ICD-10 Code | Condition Group |
G70 | Myasthenia gravis and other myoneural disorders |
G71 | Primary disorders of muscles including muscular dystrophies |
G72 | Other and unspecified myopathies |
G60–G64 | Hereditary and idiopathic peripheral neuropathy |
G12 | Spinal muscular atrophy and related syndromes |
Understanding the correct neuromuscular disorder ICD 10 classification helps families navigate insurance claims, therapy referrals, and specialist consultations more confidently.
What Causes These Conditions?
The reasons behind these conditions can be different for every child or adult. Some are present from birth, while others develop later because of illness, immune changes, or nerve and muscle damage.
Genetic Mutations — Some conditions are passed through families or happen because of changes in genes. Examples include Duchenne muscular dystrophy and spinal muscular atrophy (SMA).
Autoimmune Conditions — Sometimes the body’s immune system mistakenly attacks healthy nerves or muscles. This can happen in conditions like Myasthenia Gravis or Guillain-Barré syndrome.
Metabolic Disorders — The body needs energy for muscles to work properly. When certain enzymes are missing or not working well, muscles may become weak or tired more easily.
Infections — Certain viral or bacterial infections can affect the nerves or trigger temporary weakness in some children and adults.
Toxic Exposure — Exposure to heavy metals, some medicines, or harmful chemicals may damage nerves over time.
Unknown Causes — In some cases, doctors may not find one clear reason, even after testing.
Why Early Testing Matters
In children, inherited and congenital causes are more common. That is why early genetic testing and developmental assessment can help families understand the condition and plan the right support.
Treatment Options
Treatment is based on the diagnosis, your child’s symptoms, and daily needs. In most cases, children do best when different therapies work together as one complete care plan.
Therapy and Medical Support
- Physical Therapy — Helps improve strength, balance, posture, flexibility, and movement skills. At PediGYM, therapy programs may include Neurodevelopmental Therapy (NDT).
- Occupational Therapy — Supports everyday activities such as dressing, feeding, writing, playing, and becoming more independent at home or school.
- Speech and Oro-Motor Therapy — Helpful for children who have difficulty speaking clearly, chewing, swallowing, or controlling oral muscles.
- Medications — Some children may need medicines to reduce inflammation, support the immune system, or treat specific conditions such as SMA.
- Assistive Devices and Orthotics — Braces, walkers, wheelchairs, splints, and communication devices can make daily life safer and easier.
- Sensory Integration Therapy — Some children also need help with body awareness, attention, and sensory processing challenges.
- Genetic Counselling — Gives families information about inherited conditions, future planning, and available medical options.
PediGYM Support Services
At PediGYM, children may also benefit from Dynamic Movement Intervention (DMI) when suitable for their goals and abilities.

When Should You Consult a Specialist?
It is a good idea to seek professional advice if you notice any of these signs in your child:
Missed Milestones — Your child is not sitting, standing, crawling, or walking at expected ages.
Progressive Weakness — Everyday activities such as climbing stairs, running, or lifting toys become harder over time.
Frequent Falls — Your child trips often, seems unsteady, or struggles with balance.
Family History — There is a known history of inherited nerve or muscle conditions in the family.
Breathing Trouble — Your child becomes unusually tired or short of breath during activity.
Early support can make a big difference. At PediGYM, our rehabilitation team focuses on helping children build strength, confidence, and independence through timely intervention.
Conclusion
Neuromuscular disorders can feel challenging for families, but progress is possible with the right care and guidance. Early diagnosis, consistent therapy, and family support can help children improve movement, confidence, and participation in daily life. With the right plan, children can achieve meaningful progress. If you have concerns about your child’s strength, balance, or development, PediGYM is here to help you take the next step with confidence.

Dr. Nitin, Founder of PediGym Child Development Center, is a dedicated pediatric therapy expert and DMI Level C Certified Therapist leading structured, evidence-based therapy programs in Faridabad and Gurgaon. Under his guidance, PediGym provides comprehensive pediatric rehabilitation focused on improving motor skills, coordination, sensory processing, speech clarity, and functional independence through personalized intervention plans.







